DNA can signal the presence of or predisposition to a slew of diseases, including cancer. The ability to flag down these clues, known as biomarkers, allows medical professionals to make critical early diagnoses and provide personalized treatments. The typical methods of screening can be laborious, expensive or limited in what they can uncover. A new biosensor chip that boasts an accurate and inexpensive design may increase accessibility to high-quality diagnostics.
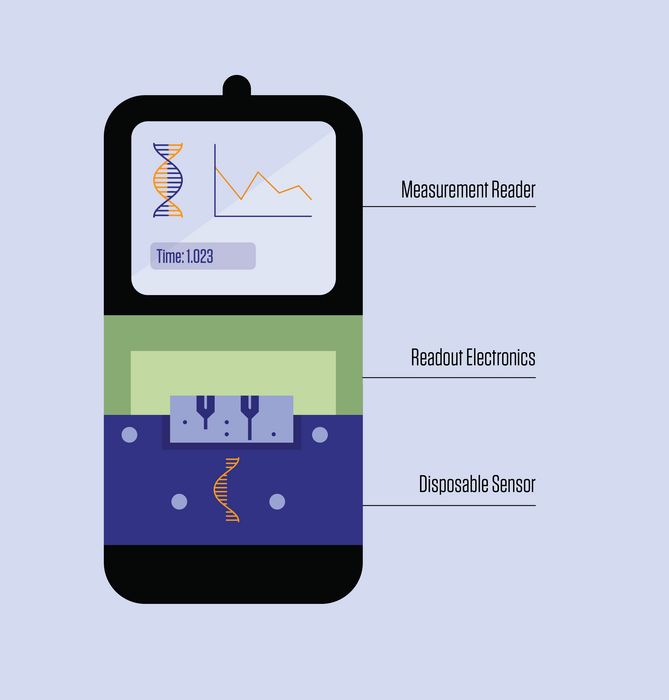
The biosensor, developed by researchers at the National Institute of Standards and Technology (NIST), Brown University and the French government-funded research institute CEA-Leti, identifies biomarkers by measuring how binding occurs between DNA strands and the device. What sets it apart from other similar sensors is its modular design, which lowers costs by making it easier to mass produce and allowing the most expensive components to be reused.
In a paper from the latest IEEE International Electron Devices Meeting just posted online, the researchers presented results of a study that demonstrates the device’s high sensitivity and precision despite its modularity, which is typically associated with diminished performance.
Like other DNA biosensors, the device takes advantage of the fact that a single DNA strand, when not paired with another within the familiar double helix, is primed for chemical bonding. Part of the device is coated with single strands of DNA. When these “probes” encounter DNA biomarkers that have a corresponding, or complementary, genetic sequence, the two strands bind, sending a signal that is picked up by the device.
“To make the measurement, we need two DNA molecules. We place one strand on our sensor that is complementary to the target DNA, that’s the proverbial needle in the haystack,” said NIST researcher Arvind Balijepalli, a co-author of the new study.
When a strand of target DNA binds to a probe, it induces a voltage shift that a semiconductor device, called a field-effect transistor (FET), can measure. These voltage shifts can occur hundreds of times a second as the molecules pop on and off the sensor.
Because of its high time resolution, this approach can tell you not only whether a DNA strand is bound to a probe, but how long it takes to connect and disconnect — a factor called binding kinetics that is key for discerning different markers that may bind to the same probe to varying degrees.
And with this method, you don’t need much space to measure a lot.
“This is a very scalable technique. In principle, we can have hundreds if not thousands of sensors in an area of one square millimeter integrated into a device the size of a smartphone, which is much less cumbersome than some of the technology currently used in the clinic,” Balijepalli said.
FET-based methods have yet to hit the mainstream, however. A significant stumbling block is their single-use nature, which until now has seemed a necessity but increases their cost.
Similar to how your radio becomes increasingly noisy as you drive away from a radio station, electrical signals also get noisier the longer they have to travel within electronics. The unwanted random noise picked up along the way makes the signal harder to measure.
To limit noise, DNA probes in FET-based sensors are normally attached to the transistor directly, which converts the signal into readable data. The drawback is that the probes are spent after being exposed to a sample, and thus the whole device is as well.
In the new study, Balijepalli and his colleagues increased the distance between the probes and the transistor so that the more expensive elements of the circuitry could be reused. The upfront penalty was that the distance could increase the amount of noise; however, there was much to be gained from the design choice, even beyond the cost savings.
“If the reader is reusable, we can build more sophisticated technology into it and get higher precision out of the readings, and it can interface with the inexpensive and disposable sensing element,” Balijepalli said.
Because they anticipated that the modular design would diminish the biosensor’s sensitivity, the researchers took a page out of the Internet of Things (IoT) playbook, which accommodates the losses associated with wireless devices. The NIST authors paired their circuitry with a specific type of extremely low-power FET developed at CEA-LETI that is used in smartwatches, personal assistants and other devices to amplify signals and compensate for the lost sensitivity.
To test the performance of their device, they placed it in liquid samples containing DNA strands associated with exposure to harmful ionizing radiation. Complementary DNA probes adorned electrodes wired to the FET. Across several samples, they varied the amount of target DNA.
The researchers found that the binding kinetics were sensitive enough to make accurate measurements even at low concentrations. Overall, the performance of the modular design matched that of integrated, nonmodular FET-based biosensors.
The next step in their research is to find out if their sensor can perform similarly with varying DNA sequences caused by mutations. Since many diseases are caused by or associated with mutated DNA, this capability is essential for clinical diagnostics.
Other studies may evaluate the sensor’s ability to detect genetic material associated with viruses, such as COVID-19, that could hint at infection.
In the meantime, the new technology could represent a viable foundation to build upon.
“There’s an opportunity to develop more sophisticated modular sensors that are much more accessible without sacrificing high quality measurements,” Balijepalli said.
DOI
10.1109/IEDM45625.2022.10019493